TELEHEALTH A CLOT-BUSTING GAME-CHANGER FOR KIWI STROKE PATIENTS
May 2018
The chance of patients avoiding permanent brain damage or disability from stroke looks set to dramatically improve, thanks to the success of a New Zealand hospital telehealth pilot now being progressively rolled out nationwide.
It’s called Telestroke –using big city neurologist expertise to provide fast support to less experienced clinicians treating stroke patients in regional hospitals after-hours.
Nine thousand New Zealanders suffer from stroke each year. How well the brain recovers is often down to swift intervention and, if required, timely administration of clot-busting thrombolysis drugs. Ideally, a stroke patient should be diagnosed and treated within the first few hours following a stroke. However, only 36% of New Zealanders are currently treated within this time frame. One challenge to timely treatment is that too often stroke victims still wait too long to call 111, plus many smaller hospitals lack 24-hour access to a neurologist or stroke specialist.
Telestroke was successfully piloted for six months in the Central Region in 2016. It resulted in a dramatic increase in stroke treatment intervention – doubling rates of stroke thrombolysis from eight to sixteen percent, the highest regional stroke intervention rate across New Zealand.
“Everyone saw what a clear difference it made to patients and clinicians bought into it enthusiastically” says Wellington Neurologist and pilot lead Dr Anna Ranta.
Seven Wellington Hospital-based neurologists were rostered on as the “hub” service, providing expert after-hours advice via video link to four regional “spoke” hospitals in Hawkes Bay, Palmerston North, Nelson and Blenheim. The Ministry of Health provided seed funding to pay for equipment and associated costs.
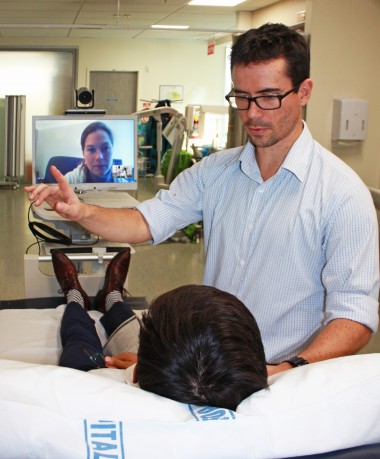
The neurologists were set up with video-conferencing and visual x-ray image systems on 4G/Wi-Fi capable iPads, while regional hospitals were provided with mobile trolley units. Once a suspected stroke patient presented at a regional hospital emergency department after hours, the local ED team triggered a ‘Telestroke alert’ to notify the on-call CCDHB neurologist. A portable unit was then wheeled to the patient’s bed for a video consultation. If clinically required, the neurologist would then support the local doctor in administering intravenous thrombolysis treatment. During the six-month trial 164 patients were assessed and 51 given the clot-busting drugs within the vital 4.5 hours.
Dr Ranta says Telestroke ensures regional patients can now consistently access the same 24/7 neurological expertise and care as city patients.
“Equity of access is so important. Why should only patients living in big cities get access to round the clock expert treatment if there are available solutions? “ she says. “If you have a technology like telemedicine, then, in my opinion, there is really no excuse not to use it”.
The CCDHB region has now adopted Telestroke permanently and since the pilot Whanganui and Wairarapa DHB’s have come on board. Other regions now look set to follow suit. The Midland DHB group, led by Waikato DHB, is establishing a similar service with Northland about to roll out its own version.
Christchurch neurologist Dr John Fink says the Canterbury DHB has also submitted a Telestroke business case and received some funding support from the Health Ministry, proposing Christchurch-based neurologists as the expert “hub”, providing support to “spoke” hospitals across the entire South Island.
Andrew Panckhurst from Mobile Health and the NZ Telehealth Forum, says it’s fantastic to see telehealth initiatives like Telestroke turning into everyday business-as-usual health solutions.
“Telehealth technology is becoming cheaper and easier to use, with medical staff showing they are increasingly likely to use video-conferencing systems like this” he says.
How does Telestroke work?
- Once a patient presents to a regional hospital emergency department after-hours with a suspected stroke, the local ED team puts in a call to have a remote on-call neurologist or stroke specialist notified.
- A portable WI-FI connected Telestroke unit (provided by Vivid Soutions) is then wheeled to the patient’s bed.
- The neurologist then uses a 4G iPad to dial into the set-up mobile unit via the secure national health network to lead a clinical team evaluation of the patient, who is then sent for a CT brain scan.
- The neurologist reviews the scan shortly afterwards via a Picture Archiving and Communication System (PACS). If clinically indicated, the neurologist can then immediately order administration of intravenous thrombolysis treatment (Alteplase)
- After the hour-long infusion, patient care is handed back to the regional physician.
